Seraccess®
Disruptive Technology for Monitoring Critical Blood Parameters
In its MedTech division, Securecell is proudly developing Seraccess®, an innovative technology that fully automates the high-frequency collection, processing, and analysis of blood using next generation microfluidics for the monitoring and controlling of critical blood parameters using the smallest blood sample possible.
Seraccess® innovation begins with an ultra precise / fully automated Glucose ICU monitor and ends with a fully miniaturized / fully mobile artificial pancreas device for personalized life-changing glucose control.
The Seraccess® Approach
The automated, regular, accurate and precise glucose measurement provided by Seraccess® will empower confident treatment decisions and lead to improved clinical outcomes. Furthermore, hospitals will benefit from significant cost reduction by eliminating manual glucose measurements.
Blood Sampling
How much blood is needed per day to measure blood glucose every 15 minutes?
The Seraccess® technology only needs 20µl to 30µl of blood to perform a measurement. At a sample frequency of 15 minutes, Seraccess® administers 96 measurements every 24 hours, which amounts to only 2ml to 3ml of blood per day.
Plasma Extraction
How to communicate directly with the blood?
One of the key elements of the Seraccess® technology is the proprietary silicon membrane, which contains millions of pores through which pure blood plasma is extracted for an accurate, precise, and nearly delay-free blood glucose measurement.
Blood Glucose Measurement
More accurate, more precise, and nearly delay-free
The photometric method used by the Seraccess® technology provides much more accurate and precise blood glucose measurements than conventional electrochemical methods, which are subject to interfering factors such as signal drift, time delay, slow response time, as well as substances such as hydroxyurea, acetaminophen, or paracetamol.
Blood Glucose Monitoring
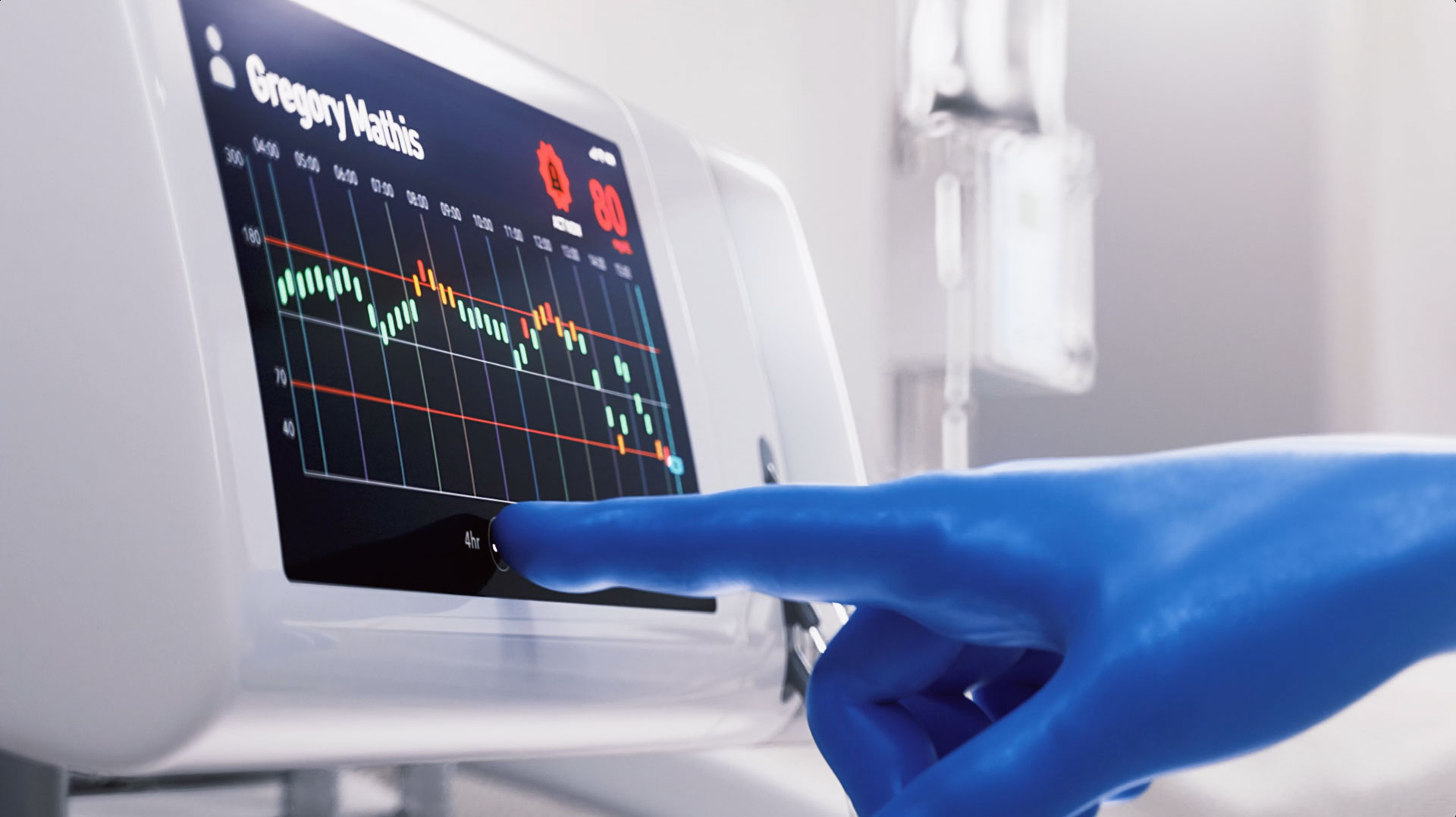
Reliable blood glucose monitoring
An intuitive, easy-to-use screen interface supports patient management. As a default, blood glucose measuring frequency is set at 15 minutes and can be adjusted as needed. Due to this increased measuring frequency, Seraccess® AXM can lead the way towards reduced glycemic variability and improved clinical outcomes.
Seraccess® Milestones
-
SERAPORT - TAKING TRANSDERMAL PORTS TO THE NEXT LEVEL
Making sampling of minute amounts of blood possible
Learn more -
THE BENEFITS OF THE INTRAVENOUS PATHWAY - PART I
Improving Time-in-Range not only in the STRECHTED RANGE (70-180mg/dl), but also in the HEALTHY RANGE (70-140mg/dl) ?
Learn more -
THE BENEFITS OF THE INTRAVENOUS PATHWAY - PART II
Does measurement delay have a negative impact on Time-in-Range (70-140mg/dl) ?
Learn more -
THE LONG-TERM RELIABILITY OF SERACCESS’ AUTOMATED DILUTION PROCESS.
Does the Seraccess® automated dilution process perform reliably in the long term?
Learn more -
THE BENEFITS OF THE INTRAVENOUS PATHWAY - PART III
How does the Seraccess® blood glucose measurement perform in healthy subjects when compared to Cobas C111?
Learn more -
THE BENEFITS OF THE INTRAVENOUS PATHWAY - PART V
How does the Seraccess® blood glucose measurement perform in healthy subjects when compared to YSI?
Learn more -
THE QUALITY OF SERACCESS®’ CONTINUOUS AUTOMATED BLOOD SAMPLING VIA AN EXISTING CATHETER. PART I
Does Seraccess®’s automatic blood sampling, including sample preparation using the silicon membrane developed and patented by Securecell, work in vitro in a regulated blood circuit?
Learn more -
THE BENEFITS OF THE INTRAVENOUS PATHWAY - PART VI
How does the Seraccess® blood glucose measurement perform in subjects with type 1 diabetes when compared to Cobas C111?
Learn more -
THE QUALITY OF SERACCESS®’ CONTINUOUS AUTOMATED BLOOD SAMPLING VIA AN EXISTING CATHETER. PART II
Does Seraccess®’s continuous automatic blood sampling work in vivo on live sheep?
Learn more -
THE COMBINATION OF CONTINUOUS AUTOMATED BLOOD SAMPLING WITH THE BLOOD GLUCOSE MEASUREMENT
Does Seraccess®'s automatic blood sampling, including sample preparation using the silicon membrane developed and patented by Securecell and the blood glucose measurement, work in vivo on live sheep?
Learn more
Disclaimer
Seraccess® is a mid-stage venture project of Securecell that offers investment opportunities to private and institutional investors.
All information and opinions contained herein have been prepared by management and its advisors and represent their assessment as of January 2022. No representation or warranty, expressed or implied, is given as to the accuracy or completeness of the contents, opinions, or projections expressed herein and no responsibility or liability is accepted. All information videos and contents do not constitute an offer to purchase securities. The website content does not constitute an invitation to buy shares under US or international law.