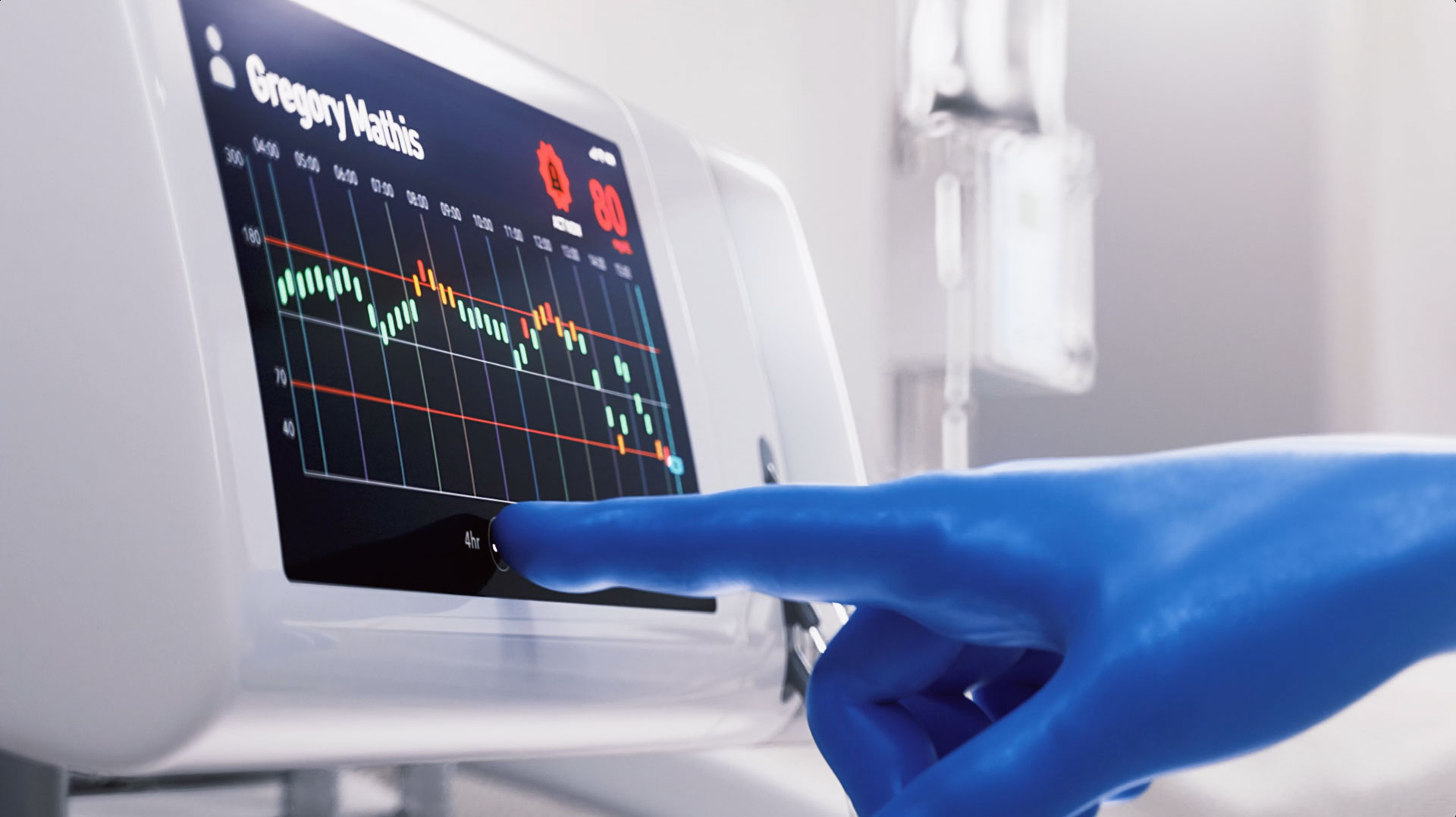
Seraccess® AXM
Automated Blood Parameter Monitoring for Hospital Care
Seraccess® AXM represents the next generation of clinical measurements offering superior analysis of glucose and beyond by combining automated blood sampling, plasma extraction and photometric accuracy to continuously monitor critical blood parameters from the smallest sample-size possible.
Why Seraccess® AXM?
Current blood parameters measurement methods, such as glucose, are mainly based on manually drawn blood samples. There are often large time intervals between measurements, and the total time needed by the nursing personnel generates significant costs.
Seraccess® AXM performs automated and regular blood sampling, using an already inserted catheter. Only a tiny amount of blood is required for each measurement and the system provides highly accurate and precise glucose values at short time intervals. Seraccess® AXM enables physicians to follow a patient’s course of blood parameters in a much closer way and empowers confident treatment decisions.
Seraccess® AXM: Monitoring Blood Parameters in ICU
Seraccess® AXM will provide nurses, doctors, and ICU personnel with a front-line tool to track patients’ physiological conditions by consistently producing 100 fully automated and highly accurate blood parameters measurements from only 2-3 ml of blood per day. Seraccess® AXM revolutionizes the way hospitals treat, e.g. dysglycemia, especially in the intensive care unit (ICU).
Avoiding dysglycemia is a key goal in the treatment of patients in the ICU.1-5 Unfortunately, both hyper- and hypoglycemia in hospitals are common and related to increased morbidity, mortality, and respectively increased healthcare costs.6 Automated glucose measurement reduces resource utilization and nursing costs, as well as length of stay in the ICU by more than a day.5,7,8 Seraccess® AXM is a system that can be integrated into existing installations to provide optimum glucose monitoring.
SERACCESS® AXM
Key Features
Seraccess® AXM - Beyond Glucose
Seraccess® AXM extends beyond glucose monitoring to deliver additional diagnostics such as lactate, sodium, and potassium analysis within one decentralized system. AXM transports the functionality of an off-line central lab to an online bedside device giving hospital workers and patients an advanced solution for the accurate monitoring of both disglycemic and critically ill patients.
SERACCESS® AXM
Blood Parameters
Opportunity
Over 200,000 beds in intensive care units in the US and Europe alone translate to a yearly potential of at least 35 million treatment days generated by about 9 million patients. An ICU bed equipped with the Seraccess® AGM durable unit will host around 100 patients per year, who will consume 200 disposable units. Overall, the value of the durable market is estimated at 1.4 bn CHF and the disposable market at 2.7 bn CHF.
Visit our Investor Relations page to contact us and learn more.
Disclaimer
Seraccess® is a mid-stage venture project of Securecell that offers investment opportunities to private and institutional investors.
All information and opinions contained herein have been prepared by management and its advisors and represent their assessment as of January 2022. No representation or warranty, expressed or implied, is given as to the accuracy or completeness of the contents, opinions, or projections expressed herein and no responsibility or liability is accepted. All information videos and contents do not constitute an offer to purchase securities. The website content does not constitute an invitation to buy shares under US or international law.
References:
1 I.B. Hirsch, L.M. Gaudiani: A new look at brittle diabetes. Journal of Diabetes and Its Complications 35 (2021) 107646; https://doi.org/10.1016/j.jdiacomp.2020.107646
2 Cryer, P.E., S.N. Davis, and H. Shamoon, Hypoglycemia in diabetes. Diabetes Care, 2003. 26(6): p. 1902-12.
3 Lind, M., et al., Glycemic control and excess mortality in type 1 diabetes. N Engl J Med, 2014. 371(21): p. 1972-82.
4 Cartwright A. et al. The outcome of brittle type 1 diabetes - a 20 year study. Q J Med 2011; 104:575-579
5 Flanagan D. What happens to people with “brittle” diabetes? Diabetes Digest 2011 Vol 10;4:196 https://www.pcdsociety.org/download/resource/2756; accessed Dec 16, 2021
6 https://www.webmd.com/diabetes/brittle-diabetes-all-about; accessed Dec 15, 2021
7 CDC National Diabetes Statistics Report 2020; https://www.cdc.gov/diabetes/pdfs/data/statistics/national-diabetes-statistics-report.pdf; accessed Dec 15, 2021
8 https://www.americanactionforum.org/research/understanding-the-insulin-market/; accessed Dec 15, 2021